March 28, 2019
Hospital Drug Diversion Prevention: Healthcare Workers Aren’t Immune to the Opioid Epidemic
The opioid crisis and hospital drug theft have been coming together in headlines for years. High-profile cases illustrate drug diversion – any time a prescription medication is removed from the intended path of manufacturer to patient – as an epidemic that’s very much alive within healthcare organizations. As a result, hospital drug diversion prevention has been a focus for pharmacy, security, and compliance departments, with efforts ranging from screening employees, limiting access to controlled substances, and closely monitoring dispensing systems.
And hospital staff are not immune to the opioid crisis. In fact, between 10-15% of healthcare workers will misuse drugs at least once throughout their careers. Establishing a drug diversion monitoring program is key for healthcare providers to prevent incidents from occurring. Without a strategy, patients, organizational reputation, and even the diverters themselves can face irreversible consequences.
Drug diversion risk: How does drug diversion affect your care?
First and foremost is the impact on patient safety. Aside from improper care and a lack of focus from intoxicated care providers, reported cases of blood-borne illnesses indicate that diverters could be infecting patients. In addition, time and resources must be dedicated to the potential of a staff member’s accidental overdose, death, and infections from improperly sterilized needles, falsified records, and theft. Investigations associated with these incidents are time-consuming and costly.
The Drug Enforcement Agency (DEA) continually examines hospital drug diversion prevention and whether facilities have a program in place. And organizations like the Joint Commission require that health systems use policies and procedures to prevent controlled substance diversion. This makes it essential to document when an incident occurs: Care providers are required to report details to the DEA, law enforcement, state pharmacy boards, and the Office of the Inspector General (OIG). All this requires extra work and effort from your team.
Discovering drug diversion and working with law enforcement to remediate instances can prevent your organization from reputational damage and sizable regulatory fines. In 2014, Mount Sinai Health System received an anonymous tip from within the organization concerning repeated incidents of drug diversion. After conducting an internal investigation, what they uncovered was extensive – one of their at-the-time Pharmacy Directors had diverted over 200,000 doses of Oxycodone throughout five years – by pilfering small amounts at a time.
“The case made headlines all over the world as far away as New Zealand,” said Bruce Sackman, former Senior Investigator at Mount Sinai Health System. “Now, could you imagine sitting on the board of directors of a hospital, opening up the New York Times, the Daily News, the New York Post, and reading this story? The good news is that we discovered it. We investigated and we brought the entire matter to the government for prosecution because if they had found it unbeknownst to us, I’m sure our fine would have been a lot higher.”
Best practices for hospital drug diversion prevention
Care providers must take a multi-layered approach to drug diversion prevention. Healthcare privacy, security, and compliance professionals should align to conduct forensic investigations to look for signs of drug diversion and identify the who, when, what, and how of drug diversion in their facility. Then, they can follow up by training and, if necessary, sanctioning employees. This helps drive a culture of security and compliance, which is important in reducing and preventing future incidents.
Drug diversion often involves unlikely perpetrators and shocking scenarios. That’s why one of the biggest tools for solving the drug diversion puzzle can be found in your very own EHR. A platform that monitors for user behavior can help detect drug diversion by spotting, for example, self-modification. Are physicians or clinicians modifying their own records to obtain medications that weren’t initially prescribed to them? Some state laws allow physicians to treat themselves, but most organizations don’t allow them to modify their own medical records. Another scenario may involve a user who reactivates a months-old expired prescription.
Automated drug diversion monitoring platforms can use trend reports and data from dispensing systems to monitor for drug diversion. These compare peer activities by title and department to reveal users who review more pharmaceutical information than their peers. In a drug diversion scenario, this might mean a user is searching for open orders and prescriptions, locating the delivery point, and picking them up using the patient’s name.
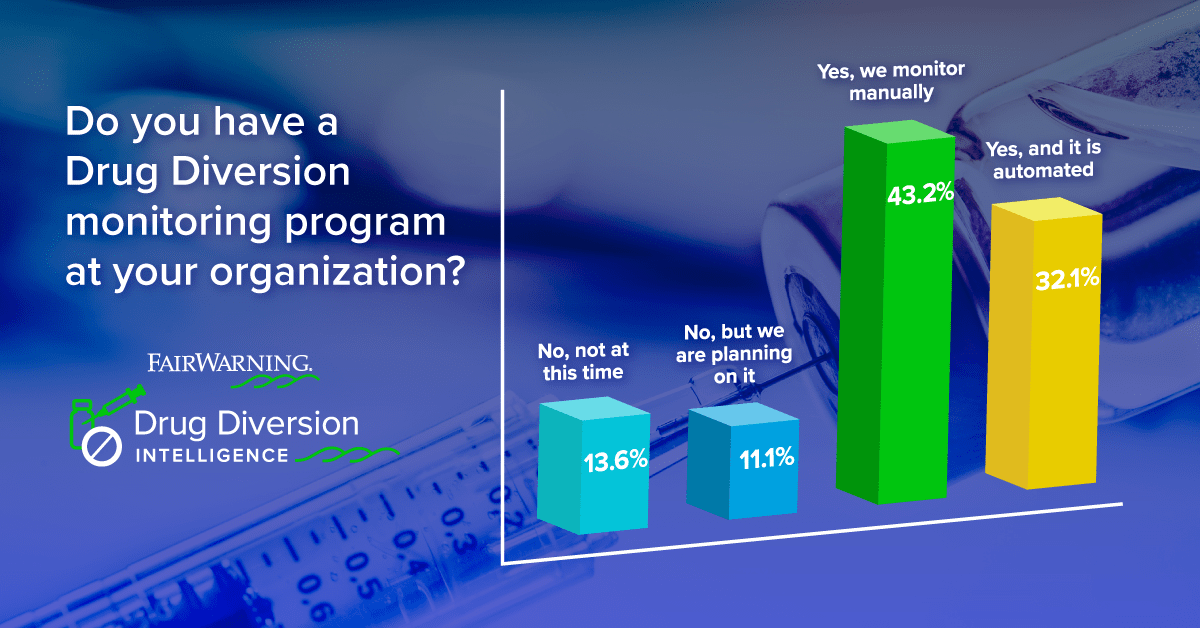
On a recent webinar, Imprivata FairWarning asked healthcare pharmacy, compliance, privacy, and security professionals whether they monitored for drug diversion. An impressive 75.3% have a monitoring system in place, but over half of those who monitor do so manually – a time-consuming process for teams without much time to spare.
Preventing drug diversion through organizational buy-in and nurturing a culture of compliance
To establish a robust drug diversion monitoring program, buy-in from leadership, boards of directors, and hospital staff is essential. And although healthcare leaders agree that drug diversion is a problem, it’s more difficult to believe that it’s happening within your own facility. Because the red flags of drug diversion often point to “gold star” workers who elect to take on extra shifts or cover the night shift, it’s challenging to identify diverters and convince members of staff to investigate other signs and signals that arise, from failure to document waste to vials that appear to be tampered with.
“In drug diversion, we see that even in fraud cases and what happens is that the managers are shocked. They can’t believe that their best employee is actually the one that wound up being the diverter.”
– Bruce Sackman, former Senior Investigator at Mount Sinai Health System
With a drug diversion monitoring program, you can attain the concrete data needed to reveal medication discrepancies to staff and leadership, enabling further investigation of potential cases. After the 2014 drug diversion incident, Mount Sinai obtained leadership buy-in, bouncing back to establish a world class drug diversion monitoring program.
“Everyone agrees that leadership engagement is the key because you want to ensure that the culture of the organization changes and that staff are empowered to come forward,” explained Lucy Cannizzaro, Associate Director of Administration & Director of Pharmacy, Director of Regulatory Affairs at Mount Sinai Brooklyn. “At Mount Sinai Health System, we have been very fortunate to have executive support for many years with a well-developed diversion prevention program in place where we had a diversion rounding program where pharmacy and compliance work together as a team to perform educational rounds.”