November 20, 2014
The Case for Smarter Clinical Workflows
The practice of evidence-based medicine can promote patient safety, increase quality of care, and improve clinical outcomes. Clinicians are increasingly being held accountable to abide by regulatory standards, Meaningful Use guidelines, and Centers for Medicare and Medicaid Services incentive and penalty programs. The move toward measuring quality and patient safety as key performance indicators in healthcare makes sense, but accomplishing these goals relies in large part upon improving efficiency.
Unfortunately, inefficiency is inherent in many of today’s clinical workflows, which detracts from the patient care process by bogging providers down and disrupting care teams’ collective thought processes. The answer is to implement technologies and processes to enable smarter clinical workflows that promote efficiency while also improving quality of care.
Take, for instance, clinical communication. As an emergency physician, I see first-hand the need for faster, more effective communications. If I am able to quickly receive information, share with colleagues, and coordinate next steps, I can better care for patients. Unfortunately, relying on pagers and other outdated technologies creates barriers that can delay care and significantly impact patients, especially in critical care situations.
Consider a heart attack patient. It is essential that providers are able to diagnose and treat the patient as quickly as possible to ensure that no permanent damage occurs. In cases of ST elevation myocardial infarctions (STEMIs), streamlining clinical workflows to speed the time from “door to balloon”—the time from patient arrival to catheterization of the coronary arteries to alleviate the occlusion—can mean the difference between complete recovery, or a life of struggling with congestive heart failure…or worse.
Cath lab activation is a coordinated effort which may involve many different care providers and care teams. This makes the workflows vulnerable to the negative impacts of inefficient communications. Consider the typical steps for the “door to balloon” process: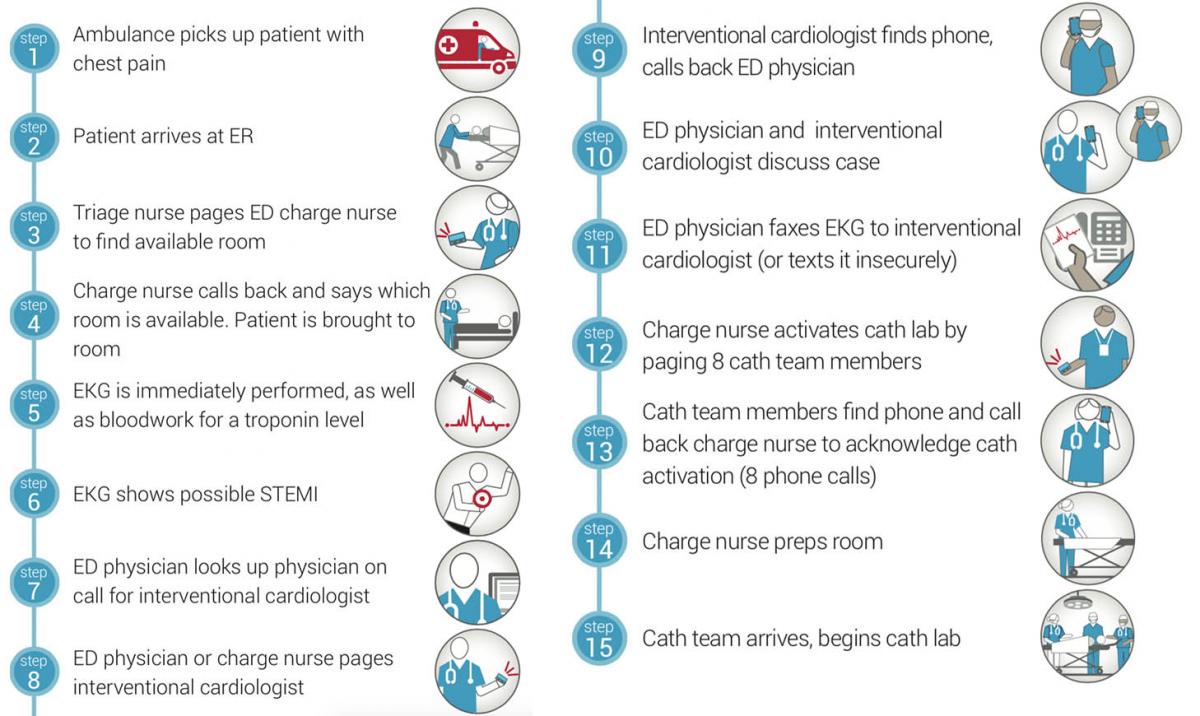
In this situation, valuable time is potentially wasted from step to step…time that could substantially impact the patient outcome. This scenario highlights the need for—and benefits of—a smarter clinical workflow. For example, if the care team could use secure communications solutions to send group messages to the care team, coordination and activation of the cath lab would be far more efficient, and the 15-step process could be reduced to just six:
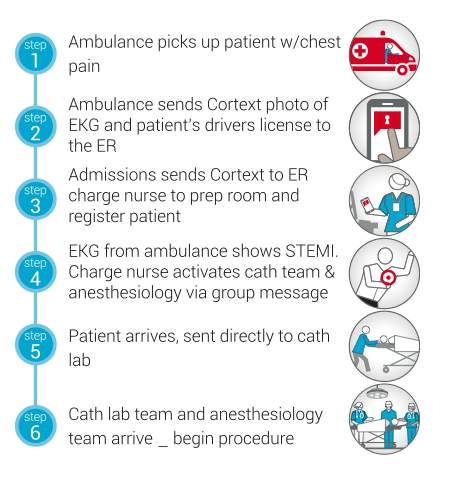
In this scenario, the smarter clinical workflow includes technology that allows:
- Immediate, synchronous, bidirectional secure messaging with the ability to send high definition images to assist in rapid diagnosis and collaboration over best treatment option (resuscitate and open up the cath lab)
- Direct integration into scheduling and on-call systems to facilitate tracking of team members, complete with read receipts, send receipts, and auditability to enable accurate, rapid messaging capabilities (ensure that the correct people are on call, aware they are on call and rapidly respond when called, complete with escalation if any delays in response)
- Group messaging capabilities to send code team activation directly to multiple devices so team members get alerted more quickly and simultaneously. Messages and responses are easily tracked and acted upon, instead of multiple pages (and waiting for callbacks)
- Multi-site communication systems to allow the notification of other clinicians needed for complete care delivery, such as the patient’s primary care physician, specialist or case manager, to provide notifications about the patient’s condition and follow-up instructions for care (which could also prevent unnecessary readmissions)
This is just one of many examples of how more efficient communication can impact the healthcare continuum. Giving physicians, nurses and other care providers the tools to do their jobs more effectively can help hospitals meet quality and patient safety goals, support accountability and, most importantly, improve the overall quality of patient care.
